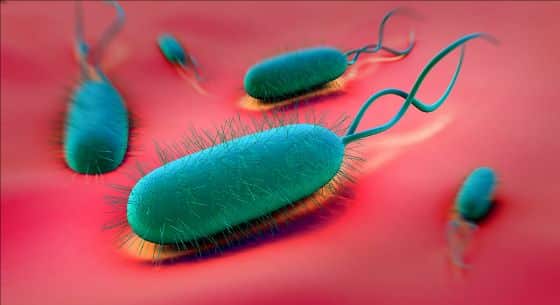
H. pylori (Helicobacter pylori) is a gram-negative bacterium that inhabits the stomach and/or the first part of the small intestine called the duodenum. It is believed that 50 percent of the world’s population carries this fella, however, not everyone develops symptoms. It can produce a broad range of upper GI symptoms like GERD, heartburn, acid reflux, a deep gnawing or burning feeling in the stomach or upper small intestine area, bloating, nausea, frequent and intense belching, and is the primary cause of ulcers and gastritis.
However, other symptoms like coughing, sore throat, loss of appetite, vomiting, weight gain, severe anxiety, chronic fatigue, joint and muscle pain, depression, brain fog with impaired cognitive functioning, and ability to focus and concentrate, can also manifest from Helicobacter. H. pylori can cause a great deal of inflammation in the stomach and the small intestine and contribute to leaky gut, which can then encourage Candida or bacterial overgrowth, and contribute to nutritional deficiencies, food sensitivities, impaired immunity, autoimmune disorders, and anything else associated with leaky gut.
Increases Gastric Cancer Risk
The World Health Organization lists Helicobacter pylori as a class 1 (definite) carcinogen, increasing one’s risk for gastric cancer significantly. However, I would like to point out that the consumption of cruciferous vegetables has been found to cut your risk for cancer by up to 54 percent. So be sure to eat lots of cruciferous vegetables if you have H. pylori.
HCL and Gastric Acid Secretion
H. pylori consume hydrogen as an energy source. The body uses hydrogen to mix with chloride to make HCL, so if this bacterium is consuming it, then you may not produce enough HCL, but it can also cause overproduction. If H. pylori colonize the area where the stomach joins the small intestine (duodenum) it can affect the cells that control HCL and result in too much HCL leading to ulceration. But, if it colonizes in the middle of the stomach, then it can impair the cells that produce HCL and inhibit production resulting in hypochlorhydria and leading to an increase in gastric cancer.
HCL is critical for digestion and protecting you from pathogenic invasion. Additionally, if you don’t have adequate HCL this often leads to a B12 deficiency, because this nutrient can’t be assimilated without HCL. Plus, HCL is what kills Candida and other microbes and keeps them from spreading through the gastrointestinal tract. Since hydrogen is H. pylori’s favorite source of energy, anything that increases hydrogen levels can exacerbate its symptoms like consuming a lot of foods that result in hydrogen production (sugar, starches, grains, carbs, fiber, fruit) and the presence of SIBO.
Although gastric acid secretion influences H. pylori, it also influences gastric acid secretion. Like Candida, the ability to colonize is dependent on pH, and in order for H. pylori to survive in the naturally highly acidic stomach, it releases an enzyme called urease, which converts urea (a substance in your stomach) into carbon dioxide and ammonia. The ammonia reduces the acidity and makes the environment more alkaline, which makes the stomach a hospitable place for H. pylori to inhabit. This alkaline environment then encourages the overgrowth of Candida and other pathogens. Additionally, ammonia is toxic to human cells and can produce a wide array of symptoms itself like confusion, brain fog, restlessness, headaches, fatigue, nausea, and even seizures or encephalitis. However, if your stomach acid is low for other reasons, (chlorinated drinking water, antacids, acid-reducing medications, poor diet, NSAIDs, steroids, pesticides, alcohol, caffeine, stress, etc) then it encourages microbes like Candida and H. pylori to multiply. H. pylori is the only bacteria known to be able to exist in the highly acidic environment of the stomach.
Toxins Biofilms and Morphogenesis
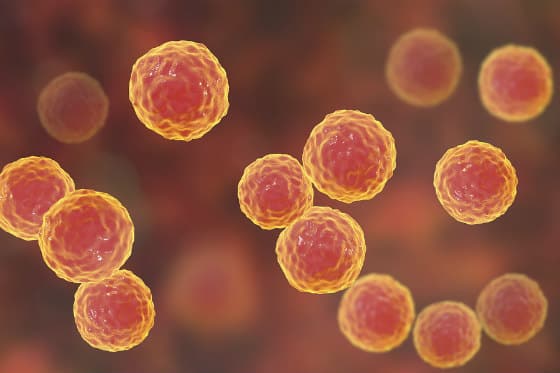
Toxins from H. pylori may lead to lower levels of vitamin C and inhibit the absorption of iron. In pregnant women, this bacteria can cause severe morning sickness. It is also able to evade the immune system because it adheres itself below the mucosal lining, which ensures its survival. Like Candida and other microbes, Helicobacter pylori also form biofilms and can morph into a different form. Typically H. pylori exist in a spiral rod shape, but when exposed to adverse environmental circumstances that threaten its survival it can change into coccoid form (resembling a coccus) that serves as a protection mechanism.
Testing for H. Pylori
Tests used to diagnose H. pylori include a blood test, breath test, stool antigen test, and endoscopy with stomach biopsy. Like all testing for microbes, there is a fair amount of false negatives. So, if symptoms suggest infection, then retest if you get a negative result or treat accordingly. The stool antigen test may be more reliable than the other methods.
Treating Helicobacter Pylori
The primary mainstream treatment for H. pylori includes two different types of antibiotics taken simultaneously with proton pump inhibitors, which is very toxic, and in my opinion, does more harm than good. Proton pump inhibitors will make the gut more alkaline, which encourages overgrowth of H. pylori and microbes and are associated with numerous problems like impaired absorption of nutrients (magnesium, calcium, and B12) that leads to deficiencies, an increase in bone fractures, weight gain, pneumonia, and overgrowth of clostridium difficile, which is very serious. This treatment protocol rarely eradicates H. pylori completely and has a failure rate of more than 20 percent.
Some of the most effective natural remedies for H. pylori include colostrum, bismuth citrate, mastica (mastic gum), zinc, lactoferrin, turmeric, cinnamon, garlic, citrus seed extract, cranberry extract, broccoli sprouts, or supplements containing their active ingredient called sulforaphane, extra virgin olive oil, berberine, vitamin C and lactic acid probiotics (e.g., L. acidophilus and Bifidobacterium bifidum). However, H. pylori frequently develops resistance to many of these substances before treatment has been thoroughly effective and it is exceptionally difficult to eliminate completely. Colostrum is also very effective for reducing the inflammation and pain associated with H. pylori.
The reason that mainstream medicine uses two different antibiotics simultaneously, is because they recognize the fact that H. pylori gets resistant very quickly to one substance when used solo, but success is increased if two are combined. The same principle should be applied when using natural remedies. A combination of substances typically needs to be used simultaneously and rotated periodically to try and prevent resistance.
Like Candida, there are different strains of H pylori, which may respond to treatment differently, so what works for one person not be effective for another. A bit of trial and error will be required and treatment typically must be repeated on an ongoing basis whenever flares occur.
On the other hand, H. pylori can hide inside yeast cells, so if Candida is present, it can provide a safe haven for them and prevent treatment from being effective.
In my own life, I had little success with the natural treatments for H. pylori, except sulforaphane. However, the sulforaphane would only keep it under control. As soon I discontinued use, it would return in full force. Mastica worked great for a few weeks, but then I got resistant. Eventually, I had to take
several rounds of antibiotics for SIBO, and at some point, I realized my H. pylori was gone. No proton pump inhibitor was needed. The antibiotics did the trick.
Diet and H. Pylori
Of course, all foods that feed microbes and impair gut integrity should be avoided when dealing with H. pylori, like sugar, grains, legumes, alcohol, caffeine, chocolate, processed foods, or high intake of complex carbs and fruit. Like most microbes, H. pylori loves sugar, which allows it to reproduce rapidly and gluten also causes high surges in overgrowth. Following a low-carb Paleo diet will support your efforts at eradicating H. pylori. Avoid overeating.
Reduce Inflammation
Nutrients and herbs that help reduce inflammation, like vitamin A, C, E, CoQ10, curcumin, and zinc will be helpful as well. Colostrum can be highly beneficial in this area as well and relieve a lot of pain.
The symptoms of H pylori can overlap significantly with Candida and even more so with SIBO. Please read this page for more details on how to help differentiate between the three of them.
References
U.S. Food and Drug Administration. Proton Pump Inhibitors Information
https://www.fda.gov/Drugs/DrugSafety/InformationbyDrugClass/ucm213259.htm
Giuliano C, Wilhelm SM, Kale-Pradhan PB. Are proton pump inhibitors associated with the development of community-acquired ammonia? Expert Rev Clin Pharmacol. 2012 May;5(3):337-44. doi: 10.1586/ecp.12.20. https://www.ncbi.nlm.nih.gov/pubmed/22697595
Azevedo NF, Almeida C, Cerqueira L, Dias S, Keevil CW, Vieira MJ. Coccoid Form of Helicobacter pylori as a Morphological Manifestation of Cell Adaptation to the Environment . Applied and Environmental Microbiology. 2007;73(10):3423-3427. doi:10.1128/AEM.00047-07. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1907093/
Olson JW, Maier RJ. Molecular hydrogen as an energy source for Helicobacter pylori. Science. 2002 Nov 29;298(5599):1788-90. https://www.ncbi.nlm.nih.gov/pubmed/12459589
Wroblewski LE, Peek RM, Wilson KT. Helicobacter pylori and Gastric Cancer: Factors That Modulate Disease Risk. Clinical Microbiology Reviews. 2010;23(4):713-739. doi:10.1128/CMR.00011-10. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2952980/
News Medical. H. pyloir bacterium produces urease to neutralize gastric acid. December 8, 2011. https://www.news-medical.net/news/20111208/H-pylori-bacterium-produces-urease-to-neutralize-gastric-acid.aspx

I had battled ulcers and other stomach problems for decades. I was finally diagnosed positive for H. pylori. Instead of conventional medicine, I took one 500 mg cranberry extract capsule in the morning on an empty stomach and took another capsule at bedtime. After a month, I was able to eat foods that I previously couldn’t. A few years later, I was tested again, and was negative for H. pylori.
Well that is fantastic Mark. However, it is quite rare that H. pylori would respond so easily without mutating. So consider yourself very fortunate.
Best,
Cynthia