We’re going to tackle this topic by answering the following question from a site visitor.
“Cynthia, my oxalate level on a recent Organic Acid Test from Great Plains Lab was 250. I don’t know if that is seriously high or not, but it was recommended that I reduce them. I cut out the spinach, severely reduced greens (but not kale) and almonds. I don’t have any idea if that has made a difference. I have so many symptoms from so many things, I don’t notice any difference when I do “indulge” in higher oxalate food. Are oxalates really harmful at that level? I hope I have reduced my level of Candida which you and I have connected on in the past, but I’m not sure about that either. Still have gas, bloating and constipation. Have been gluten-free since 2007 and tested negative recently for SIBO.” ~Lynne
Hi Lynne,
Okay, before we answer your question, let’s be sure everyone knows what an oxalate is and why it’s important.
Oxalates are a type of organic acid that occurs naturally in plants, animals, and humans. Under certain circumstances, in the human body, high levels of oxalate can form sharp, razor-like crystals. These crystals can deposit in various places throughout the body like the bones, kidneys, eyes, muscles, blood vessels, heart, lungs, sinuses, gastrointestinal tract, and brain and cause pain and inflammation, and a wide array of symptoms.
Excessive oxalates can be a contributing factor to fibromyalgia, arthritis, vulvodynia (vulvar pain), kidney stones, chronic fatigue, depression, bladder pain and painful urination, interstitial cystitis, gastrointestinal distress, hives, Zellweger syndrome (a metabolic disorder that causes mental retardation and metabolic problems), autism and other developmental disorders, thyroid disorders, and much more. In the gastrointestinal tract, they can also inhibit the absorption of certain nutrients like calcium, magnesium, and zinc, which can lead to deficiencies in these nutrients. It may also alter pH and antioxidant levels. In the skeleton, deposits “tend to increase bone resorption and decrease osteoblast” (build bones ) activity, so it could contribute to osteoporosis. In the bone, oxalate deposition may also “crowd out bone marrow cells” which can lead to anemia and immunosuppression. Deposits in the heart can tear tissue as the heart contracts.
If they deposit in the eyes, it can cause severe eye pain, which may result in eye-poking behavior, commonly seen in the autistic population. The oxalate crystals can combine with iron, decreasing iron levels that are needed for the formation of red blood cells, increase oxidative stress and damage surrounding tissue, and interfere with the transportation of glutathione. They may also attach to heavy metals like mercury and lead, carry them into the tissue, and keep them trapped. Once an oxalate attaches to a metal, it is insoluble, so this prevents metals from leaving the body. In the mitochondria, oxalates can impair energy production, resulting in chronic fatigue. There has been a great deal of success in reversing vulvodynia with a low-oxalate diet in addition to treatment for Candida.
Children with autism have a significantly higher level of oxalates in their urine than the general population, and a low-oxalate diet has shown great improvement in many associated symptoms including improvement in cognitive skills, motor skills, social interaction, speech, and much more. In the autistic population, their levels of oxalates are often as high as someone who has hyperoxaluria, even though they don’t have a genetic disorder. It is believed this is due to Candida overgrowth because treatment with an antifungal will lower their oxalate levels.
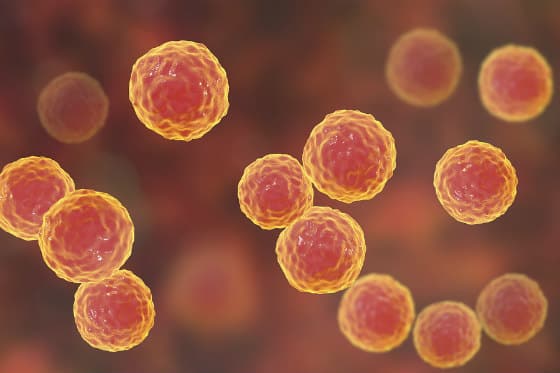
Oxalates take on different shapes depending on which metal they bind with. Although, they most commonly bond with calcium in which they may resemble a star, needles, a wedge, arrows, an envelope, or coral to name a few, they may also bind with any metal including iron, zinc, magnesium, and cobalt. Cobalt oxalates are shaped like a spear, while zinc oxalates are very thin and sharp discs. Calcium oxalates are depicted in the image above to give you a general idea of how ouchy they look – can you imagine these in your eyes, heart, brain, etc?
What Causes Excess Oxalates?
Oxalates are not inherently bad, in most cases, the body is equipped to get rid of them effectively. Like most things, it is about balance; it is when they become excessive that problems arise. There are a variety of factors that may contribute to the issue of imbalance.
- Since a lot of kidney stones contain calcium, many people are under the impression that calcium should be avoided if they have kidney stones, but according to Great Plains Laboratory, the exact opposite is true. When calcium is consumed with high oxalate foods, it combines with the oxalic acid in the intestines to form insoluble calcium oxalate crystals, that are carried out through the stool. So this form of oxalate is not absorbed by the body. On the other hand, if calcium is low in the body, then the oxalic acid in the gastrointestinal tract is soluble and is readily absorbed by the body. Therefore, adequate calcium levels are crucial for binding to and eliminating excess oxalate.
- Oxalates are formed in very high numbers by molds and fungi like Aspergillus and Penicillium, and it is believed to occur with Candida as well because Candida has been found surrounding the oxalates within kidney stones and autistic children with high oxalates can lower their oxalate levels with antifungal treatment. Therefore, individuals with Candida overgrowth or infection with Aspergillus may develop higher levels. An elevation of the organic acid, arabinose, on the OAT test often accompanies high oxalates, when yeast is present. However, even if your Candida markers are low, do not rule out a Candida diagnosis. As far as lab tests go, the Great Plains OAT test is the best tool there is for diagnosing Candida and the one I recommend. However, Candida is a master at evading detection, so a negative lab test does not mean Candida is not present.
- When there is inflammation in the gut, then more oxalate is absorbed. Inflammation may be caused by Candida, bacteria, parasites, consumption of grains, legumes, sugar, caffeine, and more.
- Vitamin B6 is a vital cofactor needed for one of the enzymes (AGXT) that break down oxalate. If B6 levels are not sufficient in the body, the enzyme will not be able to do its job adequately. Deficiency in vitamin B6 is very common.
- When lactobacillus and bifidus are low, then more oxalate is absorbed. Normally our gut flora like lactobacillus acidophilus and bifidobacterium consume oxalate and turn it into a less harmful substance and then it is eliminated through the stool. On the other hand, high levels of oxalate can kill Lactobacillus acidophilus and since high oxalate alters pH and antioxidant levels; which means gut problems can cause high oxalates, but high oxalates can cause degradation of the gut. Another particular type of organism called oxalobacter formigenes that lives in the colon relies solely on oxalate for its energy. One study found that adequate colonization of oxalobacter was associated with a 70% reduction in risk for developing a recurrent oxalate kidney stone. Therefore, insufficient numbers of this organism may encourage elevated levels. Oxalobacter formigenes can be found in some specialized forms of probiotics and may be used to reduce oxalate levels.
- Leaky gut allows oxalates to break through the gut barrier and be absorbed in higher numbers.
- Fructose is converted to oxalates, so high levels of fructose may contribute.
- Too much fat in the diet can contribute to elevated levels of oxalate if the individual is not absorbing fatty acids properly, such is the case if there is a bile salt deficiency. Fatty acids that aren’t absorbed inhibit calcium’s ability to bind with oxalates, which is needed to move them out through the stool. Bile salt may be deficient for a variety of reasons, including taurine insufficiency, SIBO, reduced function of liver or gallbladder, antibiotics, insufficient gut bacteria, some pharmaceutical medications, low pH, and genetic impairments. Additionally, oxalates oxidize your fats, making them rancid.
- High levels of the omega-6 fatty acid, arachidonic acid, are also associated with elevated levels of oxalate deposition, so maintaining a balance between Omega-3 and Omega-6 is important. The amino acid arginine can help prevent deposition.
- There are two different types of genetic variances that can impair one’s ability to metabolize oxalates, known as type 1 hyperoxaluria and type 2 hyperoxaluria; both can be fatal. Type 1 hyperoxaluria involves a deficiency in an enzyme called AGXT, and type 2 involves a deficiency in an enzyme called GRHPR. If glycolic acid is elevated in addition to oxalate on the Organic Acids Test, this indicates the presence of the type 1 AGXT genetic variance. However, these can also be elevated with a B6 deficiency as well. Elevated levels of glyceric acid in addition to an elevation in oxalates on the OAT test indicates the presence of the type 2 GRHPR genetic variance. High oxalate without high levels of glycolic acid or glyceric acid, rules out a genetic cause for the elevation.
- Ethylene glycol, the main component in antifreeze forms oxalates. As a matter of fact, it is the formation of oxalates that makes antifreeze poisonous. Ethylene glycol may be found in some foods, beverages, cosmetics, toothpaste, and other personal care products, and nutritional supplements. Oxalates are a metabolite of a variety of other environmental pollutants as well.
- In the body, decomposing vitamin c can also form oxalate metabolites during transport and storage. However, it is critical to be aware that this typically only occurs at very high doses (more than 4 grams per day in adults). Additionally, in a very large study of 85,000 women, there was no correlation between kidney stones and vitamin C intake. An evaluation performed by Great Plains Laboratory on 100 autistic children found nearly no correlation between vitamin C and oxalate levels in the urine. High doses of vitamin C have been found to significantly reduce the symptoms of autism. Since vitamin C can be highly beneficial for many of the conditions that may accompany high oxalate levels, one should not really be concerned about supplementing with vitamin C unless exceeding the 4 grams per day. However, fungi like Candida and Aspergillus can also produce vitamin C, which may cause elevated levels of vitamin C in the body; which is something to be aware of, but an elevation in vitamin C would show up on the OAT test as well. It’s also important to be aware that vitamin C can be converted to oxalates excessively if there are high levels of free copper in the body, so one would want to assess their copper levels. High copper causes vitamin C breakdown. The same is true for excess iron.
- Surgery of the small intestine and pancreatic insufficiency may also contribute.
- It’s also important to stay hydrated to help eliminate oxalates.
- A vegetarian diet (spinach, nuts, and soy protein in many meals) is very high in oxalates, so they are at a much higher risk.
Many practitioners may use calcium citrate supplementation with meals to help reduce oxalate levels, because the calcium absorbs the excess oxalates and moves them out through the stool, and the citrate competes with the oxalates for absorption. However, please be aware that if the individual has an excess glutamate problem in addition to elevated oxalate levels, this could be highly counterproductive. Calcium increases glutamate levels. Magnesium citrate may also be used, but if the dose is too high, it produces diarrhea. Intravenous magnesium can dissolve oxalates.
Test for Oxalates
You can test your oxalate levels yourself, determine if a genetic issue with oxalates exists, look at your vitamin C and B6 levels as well, and assess for Candida and Aspergillus overgrowth with the Great Plains OAT Test. This test also provides with you an abundance of other information about your health, like ammonia and D-lactate levels, bacterial overgrowth, methylation, and more.
High Oxalate Foods
According to Dr. William Shaw, founder of Great Plains Labs, about 50 percent of your oxalates come from within your own body and the other 50 come from the food you eat. If one is consuming a diet that is high in oxalates, especially if they have any of the aforementioned issues, then this can increase levels in the body. Therefore eating a low-oxalate diet can help lower the levels.
Oxalates are present in a wide variety of foods to varying degrees, but the following foods contain the highest levels.
- spinach
- beets and beet greens
- swiss chard
- collards
- parsley
- chocolate/cocoa
- peanuts
- wheat bran and germ
- tea
- cashews
- pecans
- almonds
- berries
- rhubarb
- sweet potato
- soy protein
- tofu
- leeksokra
- lemon, lime and orange peel
- quinoa
- black pepper
- instant coffee
- sesame seeds
- kiwi
- figs
- potatoes
- tangerines
- carrots
- summer squash
- celery
- summer squash
You can find a more complete list of high oxalate foods by clicking here.
Cooking your food can reduce oxalate content, but how much is eliminated depends on the method of cooking. One study found that oxalate content was reduced by 30 to 87% by boiling while steaming reduced it by 5 to 53 %. It will also help reduce phytic acid, which can inhibit the absorption of minerals. I typically recommend steaming over boiling, because boiling results in loss of nutrient content, while steaming does not. However, if one is trying to lower a really high oxalate level, then a brief period of boiling over steaming would be acceptable. In contrast, raw foods will contain much higher levels of oxalate, so should be restricted in the individual trying to bring numbers down.
Finding Your Oxalate Threshold
Now, if you are already following the low-carb Paleo diet as I hope you are, then many of the foods in this list will already be eliminated, like chocolate, soy, coffee, wheat bran and gram, peanuts, tea, and potatoes. However many Paleo-friendly foods that provide nutritional value are on this list. Therefore, you don’t want to eliminate these foods if you don’t have to. Like many other aspects of food, including FODMAPs, glutamate, or histamine issues, addressing high oxalate is about finding your unique threshold and moderating. You don’t necessarily have to remove all these foods, it depends on how high your levels are, the severity of symptoms, and how much you can tolerate comfortably. One person may tolerate more than another. Some foods may be completely off-limits, while others may be acceptable in small amounts or for a certain period of time. It’s a matter of accumulation, ability to eliminate, and other conditions that may be involved. For example, I can eat spinach with no problem for a day or two, but if I eat spinach for 3 days or more consecutively, then I begin to develop severe pain in my eyes from what I assume are oxalate crystals. However, my oxalate level on the OAT test was not elevated, again pointing out that lab tests are not always reliable.
Back to Lynne’s Question
So to come back now to Lynne’s question we presented in the opening paragraph. Anything over 101 on the Great Plains Organic Acid Test for oxalate is considered elevated, so Lynne, your number of 250 is pretty high. As discussed above, this could potentially cause a lot of problems. Unfortunately, when one has a lot of different issues going on, it can sometimes be difficult to determine whether they are seeing any improvements. Additionally, there can be a worsening of symptoms as one goes through a period of dumping oxalates when they are elevated. If I were you, I would do as you did and engage in a brief period of serious restriction of oxalates to get that initial number down to a lower level. Then from there, I would just moderate the foods to help maintain the balance. I wouldn’t eliminate them completely. However, be sure to note whether your glyceric or glycolic acid are elevated as well; as mentioned above this indicates a genetic problem, which may require more moderation.
Considering the fact your oxalate level is so elevated, it is highly likely your Candida may not be significantly reduced. However, your elevation may be due to any of the other factors presented above, so be sure to explore those and see what applies to you. In most cases, keeping Candida under control requires lifelong vigilance. If your Candida markers are elevated on the OAT test, then this would be the reason for the elevation in oxalates for sure. However, even if your markers for Candida are not elevated, that doesn’t mean Candida is not still a problem. As mentioned previously, it is very common for Candida to evade detection.
Additionally, if you continue to have constipation, gas, and bloating after following a low-carb Paleo diet faithfully, this suggests that there is likely a SIBO problem. Even though you tested negative on the SIBO test, that does not mean you don’t have SIBO. The SIBO test produces a very high number of false negatives, especially if performed with glucose instead of lactulose. I encourage you to read the three SIBO sections of my site found here, here, and here, and proceed accordingly. You can’t rely on lab tests alone when it comes to microbes, because our lab tests for this purpose are not very reliable. The best way to test for microbes is with one’s case history, past and present symptoms, and the response one has to treatment.
References
Dr. William Shaw. The Role of Oxalates in Autism and Chronic Disorders
Dr. William Shaw. Oxalates: Test Implications for Yeast and heavy Metals
Great Plains Laboratory – OAT Test
Kaufman, D. W., Kelly, J. P., Curhan, G. C., Anderson, T. E., Dretler, S. P., Preminger, G. M., & Cave, D. R. (2008). Oxalobacter formigenes May Reduce the Risk of Calcium Oxalate Kidney Stones. Journal of the American Society of Nephrology : JASN, 19(6), 1197–1203. doi:10.1681/ASN.2007101058 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2396938/
Chai W1, Liebman M. Effect of different cooking methods on vegetable oxalate content.J Agric Food Chem. 2005 Apr 20;53(8):3027-30. https://www.ncbi.nlm.nih.gov/pubmed/15826055
University of Pittsburgh. Low Oxalate Diet https://www.upmc.com/patients-visitors/education/nutrition/pages/low-oxalate-diet.aspx
Calcium Oxalate Image – By Kempf EK (Own work) [CC BY-SA 3.0 (https://creativecommons.org/licenses/by-sa/3.0)], via Wikimedia Commons


Re: calcium to reduce oxalates
Even though I have osteoporosis, I was not taking supplemental calcium until I read that it could help reduce oxalates. (mine were 250). I started taking a 1:1 citrate combination of calcium magnesium powder (I need the magnesium for constipation). Since then, however, I have read that calcium/magnesium should never be taken together as they conflict. Is that true? Would that apply to an organic whole food multi vitamin? Do you have a blog post on the topic of oppositional effects of vitamins and minerals?
Many thanks.
Hi Lynne,
Calcium should not be taken without magnesium. Too much calcium will cause depletion in magnesium and magnesium is critical for numerous reasons. Additionally, excess calcium without mag is going to cause an excess in glutamate, which is going to cause a great deal of anxiety and other negative symptoms. I don’t know what the dosage would be in whole food vitamins, but yes, it would still apply. No, I don’t have an article on oppositional effects.
The best way to address constipation until the underlying cause is identified is with high dose buffered vitamin C powder.
Take a look at Dr. Shaw’s article where it discusses using magnesium to lower oxalates.
https://www.westonaprice.org/health-topics/the-role-of-oxalates-in-autism-and-chronic-disorders/
Best
Cynthia
I live in S. California specifically in San Bernardino county. I have high oxalates, celiac disease, lyme,mold, and Candida. Is there anyone in my area who can help me with my diet. I am very sensitive and can not do
medicine very well. Is there some one on the internet or by phone who can help me? Sally
Hi Sally,
I offer consultations by phone. Info can be found here
https://www.holistichelp.net/integrative-holistic-health-coaching/
Hi, I stumbled upon your article and had a question for you. I am a avid runner but have suffered mightily the past two years. This past winder/fall I developed over 12 kidney stones with issues that lasted around 8 months. The past few months have been ok but again my speed and stamina have taken a major hit. I feel bloated a lot with gas issues and groin discomfort. Also, dizzy in the mornings and back aches with nausea off and on. Last week I had a two hour run where the entire time my stomach was bloated and very painful. Then this week I had three days of bowl issues and nausea. The doctors keep telling me nothing is wrong but I feel off. I even had my fist curl into a ball and I started yelling so they had to stop taking my bp. So far the only thing that appears off is my nephrologist said I had a high oxalate count and may need medication. Could this really the root of my issues?
Hi Paul,
Sounds like you may be exercising too much. You may want to take a look at this page.
https://www.holistichelp.net/blog/are-you-getting-too-much-exercise/
Plus, you may have developed a gut condition. You may want to take a look at these pages.
https://www.holistichelp.net/blog/sibo-101-a-comprehensive-guide-to-small-intestinal-bacterial-overgrowth/
https://www.holistichelp.net/blog/sibo-treatment-diet-and-maintenance/
https://www.holistichelp.net/blog/candida-sibo-or-h-pylori/
Hi Thanks for the article. Interesting that fungi can make vite C. Had read on Susan Owens trying low oxalate site , that candida doesnt make oxalates. Is there references for what makes oxalic acid? Am trying to find the balance and noticed in past trouble with glutamates, histamine, oxalates…
I slowly reduced oxalic acid foods (read some have major problems reducing too fast), and had bad histamine type reactions. Also had trouble taking calcium and B6. Am wondering what snps might show have possible hyperox problems. Guess to see whats going on the Great Plains test might be useful.
Hi Lynn,
As discussed above, Candida has been found in kidney stone oxalates, and autistic children can lower their oxalate levels with antifungal treatment, and Candida markers and oxalate level markers are associated, so it is believed that Candida can elevate oxalate levels, like other molds and fungi. At the end of the article, there is a list of references, please take a look at those for more information. And yes, you can test your oxalate levels yourself on the following page.